Every year, about 1 in 7 facilities fail American College of Radiology (ACR) mammography accreditation. That’s roughly 13% to 14%! Here’s the part that is really scary... About 92% of those failures are due to clinical image deficiencies and technologist positioning.
Wait. What?!
We as technologists review and select our best images, and then our radiologists choose the best of those to submit. So how is this still happening?!
Even some of the top breast centers have failed, not often, but it happens. When it does, it's not just frustrating, it's expensive. A clinical image failure can cost a facility thousands in reapplication fees, corrective action, and additional required training. Not to mention the time, stress, and impact on team morale.
Here’s the bigger issue. . .
While no change can guarantee you will avoid regulatory scrutiny, proactive improvements absolutely strengthen image quality, especially when it comes to positioning. Research published in the American Journal of Roentgenology (1) supports this. According to the U.S. Food and Drug Administration, poor positioning reduces the sensitivity of mammography by 18.1%. That means we miss more early cancers when positioning is not optimal. That number alone should be the motivation for change and the desire to be proactive in your approach to providing the highest quality care for our patients
This is not just about passing accreditation. It's about protecting our patients and delivering the highest standard of care every single day. This means we must optimize image quality so we don't miss cancers.
So the real question is not whether failures happen...
The real question is whether or not we're going to wait and react. Or are we going to lead and be proactive?
Proactive Changes
Standardized Positioning Techniques
We already know positioning is where most facilities get into trouble. The good news? It’s also where we can make the biggest impact.
Updated, standardized positioning techniques for both Full-Field Digital Mammography (FFDM) and Digital Breast Tomosynthesis (DBT) truly improve image quality. The challenge is that the original ACR Manual was written in 1999. That was before FFDM and DBT became the norm. Positioning improvements were needed to accommodate equipment changes: wider, thicker and longer image receptors (IR), and increased size of the tube head and face shield.
That’s one of the important reasons that The Miller Method™ was developed. It addresses the realities of modern equipment and has been supported by data showing measurable improvement in positioning quality. We share many free resources on our website because everyone deserves access to better tools.
That said, the real transformation often happens during and after on-site positioning training.
There are no online courses, videos or books that can replace hands-on training. With Mammography Educators on-site training, expert trainers come to your facility and work with you in your clinic environment using your own equipment and with your own patients. And the most powerful part? You can immediately see the difference.
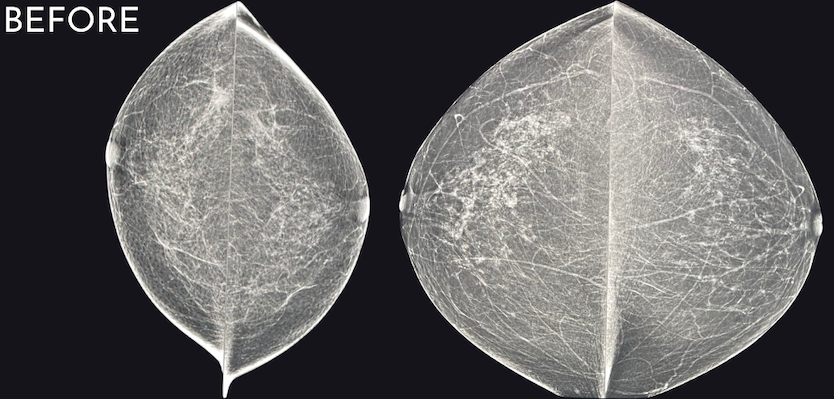
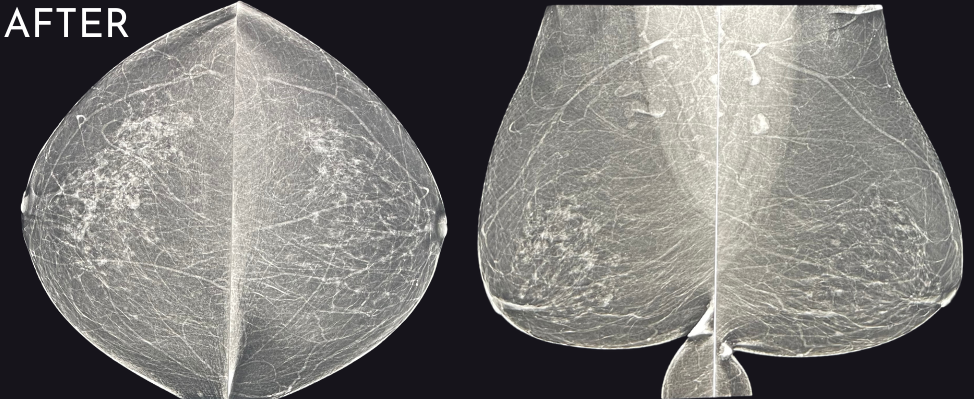
When comparing “before” and “after” images, the improvement can often be startling, even if the original images were really good! We have even identified cancers that were not visualized the year prior. Now that is amazing!
There is another benefit that doesn’t get talked about enough. The Miller Method™ is ergonomically sound, which means you're learning how to avoid positioning related injuries. While we can't go back in time, we can help reduce the possibility of new injuries. Many experienced mammographers often tell us they're dealing with wrist, shoulder, neck, and back pain. If you are a new technologist, this is your chance to build strong habits from the beginning to protect yourself from similar injuries.
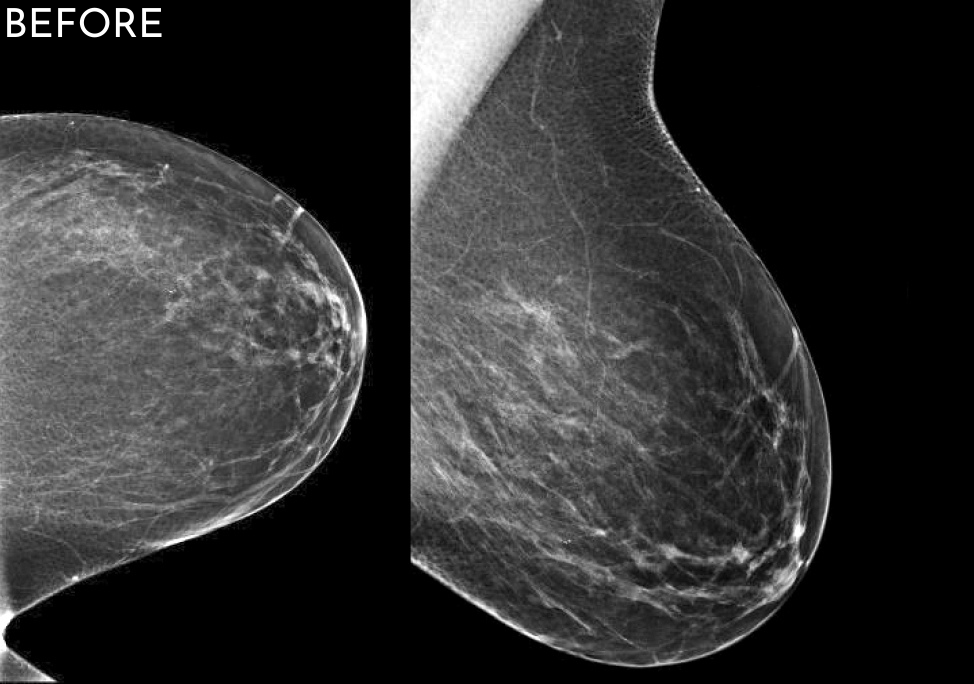
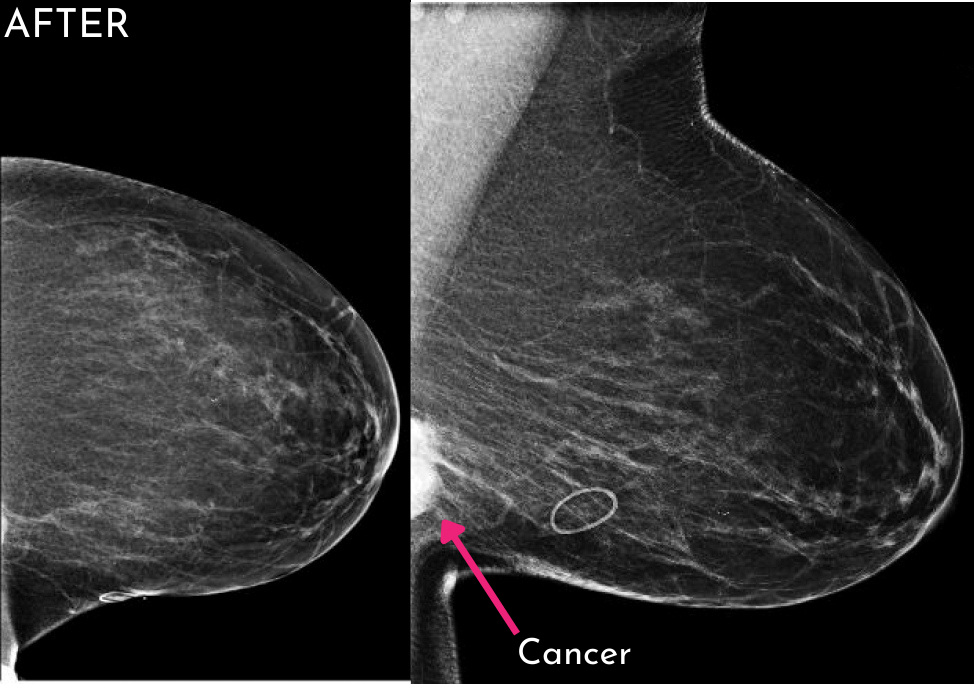
Image Evaluation
Let’s be honest, most of us assume image evaluation is something we already know how to do well. Yet images we feel confident about and radiologists approve will still fail accreditation.
The ACR provides very specific clinical image criteria, and it is important to access and throughly review this information. We offer free image evaluation sheets to help guide your assessments so you're not left guessing.
One of my challenges as a younger technologist was that while I did know what my images were supposed to look like, I didn't really know it they were “measuring up” and I wasn't unsure how to “fix” them! That is where practical education makes all the difference. It is one thing to recognize a problem. It is another to confidently correct it.
There is even variability in how the posterior nipple line (PNL) is measured. Learning the correct method, as described by Dr. Stamatia Destounis, Chair of The American College of Radiology (ACR) Breast Imaging Commission and one of the leading experts in breast imaging, can help eliminate confusion and improve consistency.
It is also important to keep expectations realistic. Even when using excellent positioning techniques, research in the Bassett (2) study shows that only about 68% of images meet basic evaluation standards on the first pass. I don’t need to tell you that we have patients that present many different challenges in terms of body habitus, breast size, shape, mobility, tenderness and other various limitations. You already know this, which is why it takes us so long to find those “perfect” images!
Even if we pass accreditation, often the reviewers will make notes regarding images, which we often think of as “dings” or criticism. It's important to recognize that comments on skin folds and/or other factors did not cause failure, but are rather just observations! If you pass, you pass, regardless of any comments that are included.
While there are never guarantees when it comes to passing or failing accreditation. There are guarantees that a proactive approach to education improves image quality and reduces unnecessary expenses. More importantly, it strengthens our ability to detect breast cancer early and provide the highest level of care for our patients. And that is always worth the effort.
References:
1) Huppe, A. et al. (2017) Mammography positioning standards in the digital era: Is the status quo acceptable? | AJR, American Journal of RoentgenologyVolume 209, Issue 6. Available at: https://ajronline.org/doi/10.2214/AJR.16.17522 (Accessed: 25 July 2025).
2) Bassett LW, Hirbawi IA, DeBruhl N, Hayes MK. Mammographic positioning: evaluation from the view box. Radiology. 1993 Sep;188(3):803-6. doi: 10.1148/radiology.188.3.8351351. PMID: 8351351.




